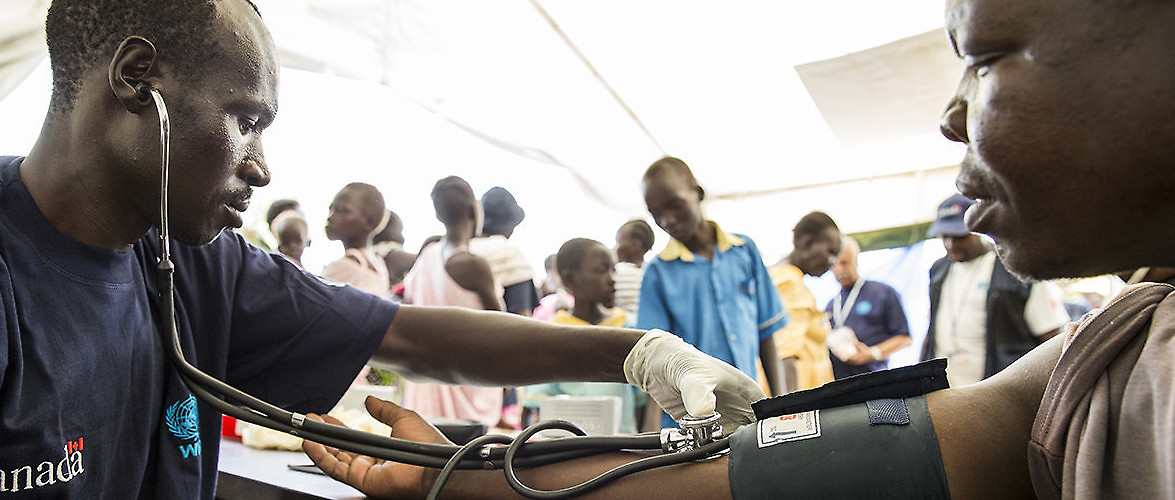
A World Health Organization official takes a man's blood pressure, as part of an UN Mission in South Sudan event. Rejaf, South Sudan, October 24 2015. (JC McIlwaine/UN Photo)
With the Zika outbreak following in the wake of Ebola as a major international crisis, global health expert Ilona Kickbusch said there is a need to better connect disease responses with concerns such as environmental and economic management.
“We need to see health, wealth, people, and planet in a much more integrated way,” said Dr. Kickbusch, Director of the Global Health Programme at the Graduate Institute of International and Development Studies in Geneva.
For one, “we have in global health focused only on people and we have not considered how the way we live—and to some extent, how our own health institutions—actually impact negatively on the health of the planet through our resource use,” Dr. Kickbusch said, on the sidelines of an Independent Commission on Multilateralism (ICM) retreat on global pandemics and global public health.
“We are dependent on the planet,” she told ICM Senior Adviser Els Debuf, “and many of the infectious disease outbreaks that we see now are linked to ecological problems.”
Also, with the United Nations’ recent adoption of the 2030 Sustainable Development Goals (SDGs), Dr. Kickbusch stressed the importance of implementing all health-related goals and targets, not just Goal 3 of good health and wellbeing. This means forming alliances to help create a healthy planet. “I think the SDGs, if we approach them correctly and not vertically—each goal on its own—creates a tremendous opportunity.”
In your keynote address, you promoted a more holistic vision of looking at global public health challenges that cuts across different sectors and different policy areas. You mentioned, for example, that we can’t separate a healthy population from a healthy planet and that health and wealth are not necessarily interchangeable. What would you say are the main challenges that need to be addressed to achieve this more comprehensive, holistic vision?
Such a comprehensive vision that links the health of people and the health of the planet is incredibly important. We have in global health focused only on people and we have not considered how the way we live—and to some extent, how our own health institutions—actually impact negatively on the health of the planet through our resource use.
Therefore, colleagues have developed a concept of planetary health, where we look at the health of people and the health of the planet at the same time and in an integrated manner.
That relates also to our understanding of wealth, of course. We see at present that there is growing wealth in the world, but that it is very unevenly distributed. The link between inequality and health is very high and much of the growth actually endangers the health of the planet. So again, we need to link in a better way the impact of our lifestyles, the impact of inequality, and the impact of a certain model of growth on our health and the health of the planet.
We are dependent on the planet, and many of the infectious disease outbreaks that we see now are linked to ecological problems. Linked to the fact that the climate is changing in areas, we have floods, we have catastrophes and emergencies. That interface is going to be more and more important; also linking humanitarian crises, health crises, and natural disasters.
It’s not a great leap to speak about the recently adopted 2030 Agenda for Sustainable Development, particularly the specific, health-related SDG, and the adoption of the new Paris agreement on climate change. How do you think these instruments can impact the current global public health debate, and how can they contribute to it? How can we achieve this very ambitious goal, SDG 3, which promotes health and wellbeing for everyone? And how can we secure the funding for interlinking public goods such as climate, health, and poverty eradication?
I think we’re headed the right way with the SDGs because on the one hand, we have one goal on health, SDG 3. Some people said we should have had more goals on health. I actually agree with that, because the Goal 3 is full of many, many health issues that we want to resolve and still misses some of them.
I suggested an additional goal on global health security, which also includes health crises and includes antimicrobial resistance as a major challenge. But what we see is that the SDG approach says, “Don’t tackle the goals separately.” Make sure that there is a clear political interface between the goals. Let me give a example of how this can work, with regard to the goal on sustainable production and consumption [SDG 12]. If you look at the growth of noncommunicable diseases, for example, this is a goal that is going to be incredibly important for health because it links to our food production. Again, it links to our lifestyles, it links to urbanization. So I think one of the important things in implementing health in the SDGs—not just the health goal—is to look at these interfaces, make sure that we address the determinants of health that we find in other goals, and find the alliances that we need to create a healthy planet.
I think the SDGs, if we approach them correctly and not vertically—each goal on its own—creates a tremendous opportunity. They are supported by other recommendations and political initiatives like the Paris agreement on climate change. It took quite some time to get health into the Paris agreement—it was not easy at all but was finally possible.
Public health services are and must be where people live their everyday life, and since more and more people live in cities—more than half of the world’s population—the activity of mayors and at city level will be increasingly important. Now, of course, how do we finance all of this? If you go through target by target, goal by goal, you get billions of dollars, and there is a fear that the goals might start to compete. Is Goal 3 more important than Goal 7? And where should the money go?
Therefore, we can see through the SDGs that we need a new mechanism to finance our progress—we call that “financing global public goods.” We need to have financing mechanisms that are reliable, that are not dependent on the old development aid model, which is starting to crumble as countries find it difficult to find the funds to continue to keep their commitments. Therefore, many of us are suggesting that we really must move forward and find a way of financing these global public goods through levies.
At national level, there can be levies on tobacco tax, for example. In the international arena, there can be levies on airline tickets—that is my own favorite. Just a couple of cents or 50 cents or a dollar on each airline ticket would allow us to respond to a lot of health crises on the one hand and on the other hand, build universal health systems and make sure that countries are prepared. Another suggestion has been to have very small levies on international financial transactions. And again, this is something that should be revisited. It was on the EU agenda at one stage, but with the financial crises, it disappeared. I think we seriously have to go back, otherwise we will not be able to respond to the interconnected crises that we face.
You mentioned that health needs to be delivered where people live. And there needs to be an investment in health at all levels. How can we invest in health and deliver on health in situations where the state itself, or part of the state, is under great stress, either due to conflict and violence, long-term development challenges, or to some of the newer challenges that have come? How can we overcome some of the obstacles in the city or state level to invest in public health?
I do believe the increase in humanitarian crises and the fact that so many people—due to war, to famine, through a whole range of population movements around the world—will not be able to rely on a state providing them basic services. This is one of the new challenges for the UN system.
I think we will have to explore what the role of the World Health Organization (WHO) is in such situations. There have been examples where the WHO has managed the health system for a country—just after the Yugoslav wars for example. We have to revisit this. It means a new type of cooperation between, for example, the WHO and the major UN agencies. Not just in crisis response—the “let’s help these people straight away with health services”—but really, in an organizational and nearly institutional response so that, until new infrastructures and new institutions can be built and a state is able to function again, people will have reliable services.
We’ve also seen that many of the refugee camps are not there for a year or two. People live there much longer, sometimes nearly for a decade now, and therefore, we do have to face the fact that there needs to be significant international funding for the health services in these camps. We cannot leave that to the countries that have taken all these refugees. They are carrying an unbelievable burden.
It is also something that cannot just be resolved through the World Food Programme and through nutrition, as important as that is. It needs a concerted effort, and I would hope that possibly another high-level panel, particularly following the two big summits we’re going to have this year—the World Humanitarian Summit and the Refugee Summit—will face up to this. I think we must use those summits to raise this issue and to find mechanisms—both institutional cooperation between agencies, many of the humanitarian actors, UN organizations—and countries willing to support this.
This interview was originally published on the ICM website. It has been edited for clarity and length.